
Irritable Bowel Syndrome
January 12, 2021
What Causes It and How to Fix It
Irritable bowel syndrome or IBS is one of the most common causes of symptoms in the digestive tract. It is estimated that 15-20% of the population have some degree of IBS. Just over 50% of all patients presenting to health care providers for digestive symptoms will receive the diagnosis of IBS.
The typical symptoms associated with IBS include abdominal pain, bloating, indigestion/reflux, constipation, and diarrhea. Interestingly different persons with IBS will have different combinations of these symptoms. This relates to the diversity of underlying problems that cause the symptoms in different people. One may have the symptoms caused by an immune inflammatory reaction to a particular food called a food sensitivity, while another may have dysbiosis, an imbalance in the microbiome or the bacteria and yeast that reside in the GI tract. The successful treatment of IBS centers on accurately determining what the triggering factors are in each case.
Triggering Factors
Food sensitivities
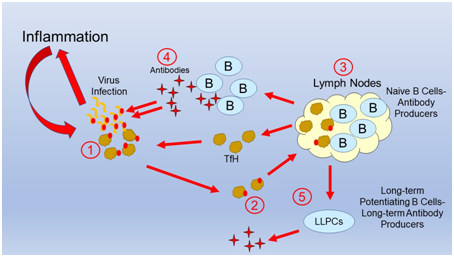
Food sensitivities are immune inflammatory reactions against a component in food such as gluten in certain grains or casein in dairy. The immune system identifies that component as dangerous the way it would to a harmful organism such as a harmful bacteria or virus. Just as the immune system would induce inflammation to begin the attack against these organisms, it will do so against a food component triggering the inflammatory symptoms.
The inflammatory symptoms may be confined to the digestive tract, or they may also involve other areas of the body such as the skin, joints, muscle, and brain. Alessio Fasano, MD, a leading researcher and authority on gluten sensitivity states that what begins in the gut (referring to inflammation) does not stay in the gut. This is not surprising as 75% of all immune activating tissue in the body is in the lining of the digestive tract. For those interested in a more in-depth discussion of this by Dr. Fasano the first 10 minutes of his lecture https://www.youtube.com/watch?v=wha30RSxE6w is educational.
The first step in resolving IBS related to food sensitivity is identifying that one exists and to exactly what food component. This can typically be done with Biomeridian testing which measures meridian reactions to different food signals. In some cases a blood test of a slow reacting antibody called IgG, against different foods in needed.
Dysbiosis
Dysbiosis is an imbalance in the microbiome living in the gut. To give a perspective how that can be such an important factor, the microbiome consisting of bacteria, viruses and other organisms is made up of 100 trillion organisms. To get a perspective on the size of the human microbiome, there are 10 cells in the body which are micro-organisms for every 1 cell of our own.
In a general sense, these organisms can be divided into “good guys” and “bad guys”. A healthy microbiome helps calm and regulate the immune system, while a dysbiotic one triggers immune inflammatory activation. As with food sensitivities, many times dybiosis can be determined with the Biomeridian test. In more complex cases a stool PCR test is done. Once the pattern of dysbiosis is identified specific antimicrobials are used to reduce the dysbiotic organisms and specific probiotics of the preferred organism are added back. A healthy microbiome helps to prevent the overgrowth of the dysbiotic organisms.
Small Intestinal Bacterial Overgrowth – SIBO
SIBO is less common than the previously mentioned causes of IBS, but none the less it is a significant cause in some. The microbiome changes composition and increases in density from the beginning of the digestive tract to the end. The highest density of bacteria resides in the large intestine with less in the small intestine. It is the movement of food through the digestive tract that maintains this population of the microbiome, less in the small intestine and more in the large intestine. If the motility or pace at which food transits through the digestive tract becomes too slow, bacteria begin to migrate back up into the small intestine.
This high population of bacteria in the small intestine causes excessive fermentation of the unabsorbed foods producing gas resulting in abdominal bloating and discomfort. This does not occur in the presence of the high bacterial count in the large intestine as most of the food has been digested and absorbed in the small intestine.
The key question in SIBO is why is the motility through the small intestine too slow? This is typically the result of imbalance in the autonomic nervous system (ANS) that controls internal functions. There are 2 divisions of the ANS, the sympathetic (SNS) and Parasympathetic (PNS). The SNS activity is referred to as “fight or flight”, while the PNS activity is “Rest & Digest”. We do not activate digestion which includes intestinal motility during stress but only when the PNS reactivates.
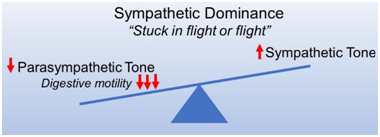
Chronic stress begins to train the ANS to stay in fight or flight, a state called sympathetic dominance. This is often hallmarked by the onset of other symptoms such as anxiety and sleep difficulty. The balance between the SNS and the PNS can be measured by a test called heart rate variability (HRV). The test measures the balance in activity between the two systems during respiration cycles. Inhalation activates the SNS which increases heart rate slightly while exhalation activates the PNS slowing heart rate. Once the balance is understood rebalancing methods such as HRV biofeedback and vagal nerve stimulation can help restore balance. The vagus nerve is the main PNS link to the digestive tract from the brain.
Occasionally, diseases can cause altered intestinal motility such as autonomic neuropathy which is a common complication of diabetes or toxicity. Those require specific testing to diagnose.
Summary
IBS is common and has different triggers. Many people who suffer from IBS have multiple triggers all which need to be explored and treated for the best outcome. In the next 3 blogs we will take each of the common triggers discussed above and cover them in more detail. IBS? The “what” to do to resolve it always starts with figuring out the “why” it is happening.